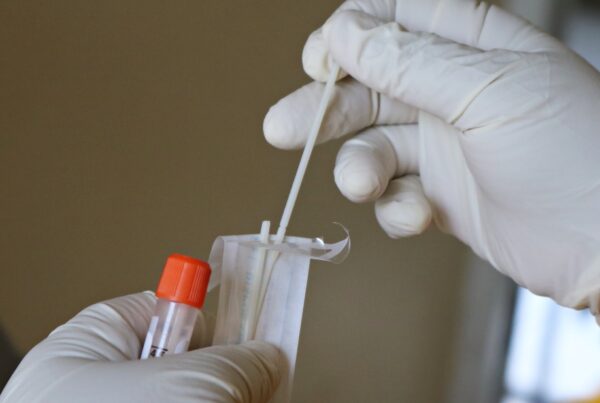
An error in the supply chain is to blame for healthcare workers’ continued practice of reusing N95 masks.
The Big Picture
An update on the number of cases and deaths from the coronavirus: As of Sunday, March 14th, the United States has over 29 million cases and 530,000 deaths from the coronavirus. North Dakota, South Dakota, and Rhode Island remain at the top of the case rate list (cases per 100,000 people), while California, Texas, and Florida still have the highest number of total cases. As of this week, over 100 million Americans have been given at least one dose of the vaccine.
With around 35 million (13%) adults fully vaccinated, Biden is calling states to make all adults eligible for the vaccine by May 1st. However, more Americans are starting to feel pandemic fatigue. With states reducing restrictions and increasing vaccinations, many individuals are relaxing personal precautions. Healthcare officials are worried that a spike in spring break travels will work against the progress this country has made.

Medical personnel don PPE before entering a COVID-19-positive, non-critical patient’s room. Flickr: Official US Navy Page
Nurses Still Reuse N95 Masks
We all remember the poignant pictures of nurses in trash bags in March of last year. But over time, as the media reported on these issues less, and people contributed to help stop, many thought the problem went away. One year later, most nurses aren’t wearing trash bags, but they still don’t have access to adequate PPE. Furthermore, they have the highest rate of death from COVID-19 among healthcare workers.
Over the past year, we have seen how unprepared hospital systems truly were for a major pandemic like this. Most nurses have been forced to continue reusing PPE like N95 masks, which quickly becomes contaminated after prolonged wear. In February, around 81% of healthcare workers surveyed by the National Nurses United stated they had reused single-use PPE. While so many nurses are aware of this problem, many haven’t been able to voice their concerns. Reports that nurses are in danger of being fired if they speak out have surfaced around the country.
Where are the N95 Masks?
N95s are critical, but there is a critical imbalance in supply and demand. Brain Wolin is one of the many Americans who decided to make a difference during this pandemic. Upon hearing about the shortage of N95 masks, he applied to get approval by NIOSH- the organization setting PPE standards for healthcare workers- to make his own masks. Upon getting approval, he expected an overwhelming amount of demand. Instead, he is now running his production at half capacity and has boxes of N95 masks laying in his warehouse.
He’s not alone. CNN spoke to 7 of the 22 new manufacturers who received NIOSH approval during the pandemic. Six out of the seven spoken to said they could not sell all their masks, and all were not “operating at their maximum capacity to make the most N95 masks possible.”
“We listened to your calls for help. And we’re here to help. So please help us help you. And as I said, we’re ready to open any way possible that we can to produce as many that would possibly be needed,” stated Wolin. If manufacturers like Wolin are so willing to help, why is there even a problem?
The answer: It’s because of our flawed supply chain.
Large hospitals prefer to use established manufacturers, meaning they have little reason to reach out to these new suppliers. On the other hand, small healthcare facilities don’t have the resources to make connections with new suppliers. Small manufacturers also have limited production capabilities. Because many of them cannot produce bulk orders, they are often turned down by large clinics and hospitals.
The new administration is looking to work with these small manufacturers, stating that federal contracts “are in the realm of possibility,” as reported in the CNN article.
This Week at Get Us PPE
Dr. Megan Ranney, and Dr. Jeremy Faust, co-founders of Get Us PPE, co-authored an article in CNN about the threat of new variants. For a long time, experts thought the COVID-19 variant B.1.1.7, may spread more easily and therefore pose a greater threat to those who become infected. A recent study attempted to conclude if this was accurate. “Around one to two more deaths occurred among those with the B.1.1.7 variant, compared to those with other strains of the virus,” explains Dr. Ranney and Dr. Faust. So while this data shows that while this variant does show an increase in mortality, it’s not widely concerning.
Dr. Megan Ranney, a co-founder of Get Us PPE, spoke in the CNN Newsroom about the definition of herd immunity. She discussed when we might potentially reach herd immunity, if/when we can start eating in restaurants again, and the continual importance of mask mandates.