As the COVID-19 pandemic continues to strike our nation, infections, hospitalizations, and death tolls rise, leaving hospitals and smaller facilities, like nursing homes and schools, with shortages of personal protective equipment (PPE). PPE shortages are being felt throughout the nation, with nitrile gloves and N95 masks being the most requested piece of PPE.
The Big Picture
The number of cases and deaths from the coronavirus increase: As of Sunday, January 3rd, the United States has over 20 million cases of COVID-19 and over 346,000 deaths. North Dakota, South Dakota, and Wisconsin maintain the highest case rates (cases per 100,000 people). However, states all across the country quickly see spikes in cases. As the holidays come to an end, NBC News reports that December was the deadliest month of the pandemic thus far. With over 77,000 deaths in December alone, it far surpasses the 58,000 deaths seen in our second deadliest month, April. This month brought hope in the form of a vaccine. The Trump administration aimed to vaccinate 20 million people by the end of December; however, only 2.8 million people have received the vaccine. Health officials cite a lack of trained staff among the many factors creating a delay. Experts also predict a surge in the coming weeks due to millions of Americans who traveled over the holidays.
Nitrile Gloves Shortage
Nitrile gloves continue to be in short supply as this PPE crisis continues. The national stockpile of nitrile gloves has dropped from 16.9 million in December 2019 to 2 million in October 2020. The US Government Accountability Office has confirmed that “availability constraints continue with nitrile gloves.” Get Us PPE’s November Shortage Index showed that nitrile gloves have already been one of the most highly requested PPE types in states like California and Illinois. Further, they are “emerging as the next major PPE shortage due to high burn rates and a disrupted supply chain.” Specifically, the price of gloves has risen to $300 per case from $30 before the pandemic. Commenting on these larger distribution issues, Dr. Ali Raja, co-founder of Get Us PPE explained, “There is still no centralized federal database for personal protective equipment. The disconnect between what’s purported to be in the stockpile and the needs on the frontline is astounding.” It is this disconnect that forces many facilities to turn to organizations like Get Us PPE for help. Although Get Us PPE has delivered over 5.5 million pieces of PPE, this amount has only fulfilled 12% of total requests. With over 78 million pieces of PPE in demand every week, it puts into perspective how dire and pressing the PPE crisis really is.

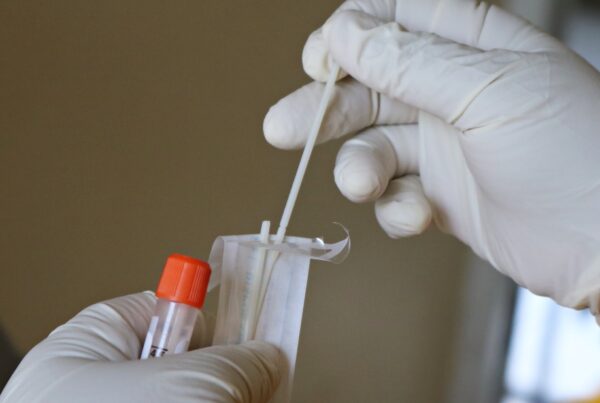
Nitrile gloves are one of the most requested pieces of PPE.
Fixing the Supply Chain and N95 Shortages
Similar trends are contributing to widespread N95 shortages. Anne Miller, Executive Director of Project N95, said that some facilities she has worked with have been reusing the same respirator for five months. Get Us PPE has collected similar data, with 86% of all healthcare workers who stated they didn’t have enough N95s were reusing masks beyond their recommended life. Many manufacturers place high minimum orders on N95s, blocking out small facilities that don’t have the funds to order thousands of masks at a time. Others prioritize large facilities that have purchased PPE from them in the past. These obstacles have contributed to increasingly unsafe conditions for all who need N95 masks. While this problem has been steadily growing in the past few months, a series of pre-pandemic events have contributed to these shortages. The Trump administration did not keep stockpiles up to date and did not purchase new technology to create N95 masks in 2018. Secondly, the administration only started purchasing orders for PPE in March, while opportunities to obtain masks had been present since January. Dr. Shikha Gupta, Executive Director of Get Us PPE is looking to learn from these mistakes as the Biden administration enters the White House. She calls for the administration to increase usage of the Defense Production Act, create price controls, and implement an “objective system for rating manufacturers so that buyers can easily see which have been vetted.”
The shortage of N95 masks will not end with the distribution of a vaccine. The New York Times recently took a more in-depth look into the PPE supply chain, and their discoveries speak to much-needed improvements in our systems. As described above, many experts have been pointing to the government’s hands-off approach to the crisis. Scott LaRue, president of ArchCare, a nonprofit overseeing nursing homes, stated, “It’s been an absolute free-for-all, and the federal government has failed to provide any meaningful leadership.” Besides governmental concerns, the markets have allowed counterfeit products to enter many healthcare facilities and price gouging to become common.
Mike Bown, the owner of Prestige Ameritech, a company manufacturing N95s, has warned the government that the American PPE system has become too reliant on foreign goods. While his company has significantly increased N95 production, he worries much of his product won’t sell. Hospitals have been shifting towards foreign manufacturers, mainly in China, producing PPE at a much lower cost. While it may be affordable, these products can often be counterfeit or set lower quality standards. Dan DeLay, an employee at CommonSpirit Health, explained that domestic PPE could be up to 40% more expensive than its foreign equivalent; therefore, it is difficult to convince healthcare facilities to invest in American-made masks.
According to research by the New York Times, “the only way to guarantee the United States has a reliable supply of high-quality masks and other medical gear is to recognize the sector as essential for national security, similar to the Pentagon’s approach for ensuring companies that make fighter jet components and military uniforms remain viable even in peacetime.”
This Week at Get Us PPE
Dr. Megan Ranney, co-founder of Get Us PPE was highlighted in nation.lk for her opinion piece on COVID-19 restrictions. As a mother, Dr. Ranney emphasizes the importance of modeling smart and responsible behavior. She explains that politicians have a responsibility to model proper COVID-19 precautions. She urges, “If there were ever a time for politicians and scientific experts to walk the walk, it would be now.” While one person traveling may not seem significant, their ability to spread the virus to those more vulnerable makes travel dangerous. More importantly, she notes that politicians and medical experts are in a unique position to set an example for everyone who looks up to them. “…I need to set the right example. I can’t ask others to do what I am not willing to do myself,” says Dr. Ranney.
Dr. Megan Ranney also spoke to MSN to detail her experience getting the COVID-19 vaccine. Upon getting the vaccine, she stated, This is the true light at the end of the tunnel. There is no better way to prevent disease than vaccination. But for it to really transform that we’re going through, we’re going to need everyone to get it.”